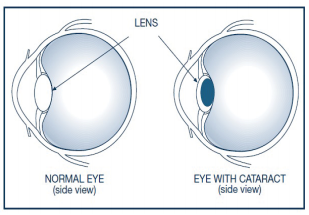
A cataract is a common eye condition where the natural lens inside the eye becomes cloudy, causing vision to gradually become blurred or dim. The lens normally functions like a clear window, focusing light onto the retina to produce sharp images, but with ageing or other factors, its proteins break down and clump together, reducing its transparency—much like glass turning foggy over time. As a result, light entering the eye is scattered rather than properly focused, leading to symptoms such as glare, poor night vision, faded colors, and difficulty seeing clearly. Cataracts typically develop slowly and painlessly, and while they cannot be reversed with medication, they can be effectively treated with a safe surgical procedure that replaces the cloudy lens with a clear artificial one.
Cataracts are not all the same—there are several types depending on where and how the clouding develops in the lens. Each type can affect vision in slightly different ways:
1. Nuclear Cataract
This is the most common type and forms in the center (nucleus) of the lens. It is strongly associated with ageing. Over time, the lens may turn yellow or brown, leading to blurred vision and difficulty distinguishing colors. Some people may temporarily experience improved near vision (“second sight”) before vision worsens.
2. Cortical Cataract
This type starts in the outer layer (cortex) of the lens and appears as white, wedge-shaped streaks that gradually move toward the center. It often causes glare, halos around lights, and difficulty with night driving due to light scattering.
3. Posterior Subcapsular Cataract
This develops at the back of the lens. It tends to progress faster than other types and commonly affects reading vision and causes significant glare, especially in bright light. It is more frequently seen in younger patients, diabetics, or those using long-term steroid medications.
4. Congenital Cataract
Present at birth or developed during childhood, this type may be due to genetic factors, infections during pregnancy, or developmental issues. Early detection is crucial, as it can affect visual development in children if not treated promptly.
5. Traumatic Cataract
This occurs after an eye injury. It can develop immediately after trauma or even years later, depending on the severity and type of injury.
6. Secondary Cataract
This type develops as a result of other medical conditions (such as diabetes) or after certain eye surgeries or prolonged medication use (e.g., steroids).
(Note: This is different from “posterior capsule opacification,” which can occur after cataract surgery.)
In general, while cataracts are a natural part of ageing, the type and progression can vary from person to person. Regardless of type, once vision starts to interfere with daily activities, cataract surgery is the only effective treatment to restore clarity.
The most common cause is growing older. Other common causes include:
You may have a cataract if you notice gradual vision changes such as blurry, foggy, or dimmed vision, sensitivity to light, or difficulty seeing at night. A professional eye exam is required to confirm the diagnosis.
Cataracts usually develop slowly and can affect your vision in different ways. Common symptoms include:
A comprehensive eye exam by an ophthalmologist is necessary to accurately detect a cataract and determine its severity. Early detection allows your doctor to plan the best treatment and timing for surgery if needed.
Cataract surgery is very safe. Although the probability of serious complications from modern cataract surgery is very low, it is important to be aware of some risks before undergoing the procedure, including:
No, a cataract cannot return once the natural lens has been removed.
In less than one-quarter of the people who have surgery, the lens capsule will become cloudy within 2 years after surgery. This is called Posterior Capsular Opacification (PCO) or ‘after-cataract’ by some. It causes the similar visual problems as a cataract. Your doctor may recommend a simple procedure to correct this problem.
Before you have your cataract surgery your general health, your vision and your eye will be checked very carefully. A biometry is done to measure the length of your eye ball and the shape of your cornea. This test help the ophthalmologist decide which lens to implant during surgery to make sure your vision is as clear as possible after the surgery.
Key preparations before cataract surgery include:
Mild redness, irritation, or slightly blurry vision is normal after cataract surgery. Seek medical attention if your eye is very painful or your vision suddenly worsens.
After cataract surgery, it’s normal to experience:
When to be concerned:
If any of these occur, contact your ophthalmologist immediately to prevent complications.
After surgery, you can usually go back to your everyday activities as soon as you feel able. There are no dietary restrictions, and you can read and watch TV as normal. In addition to taking eye drops, you may need to follow the following instructions for the first 1 to 2 weeks:
You also need to take extra care when it is windy or dusty outdoors, in case something blows in your eye, but you don’t need to stay indoors. Wear a pair of wrap-around sunglasses for extra protection outdoors.
You should typically wait 4 to 6 weeks after your eye operation before getting a new prescription for glasses. This period allows your eye to heal fully and your vision to stabilize. A follow-up eye test, known as a refraction, is usually scheduled during this time to determine your final prescription.
Why do I need glasses after Cataract Surgery?
While modern lens implants are designed to provide clear vision, you may still require glasses for the following reasons:
Where should I go for my eye test?
Once your eye has stabilized (usually 4–6 weeks post-op), you can have your refraction test performed by: